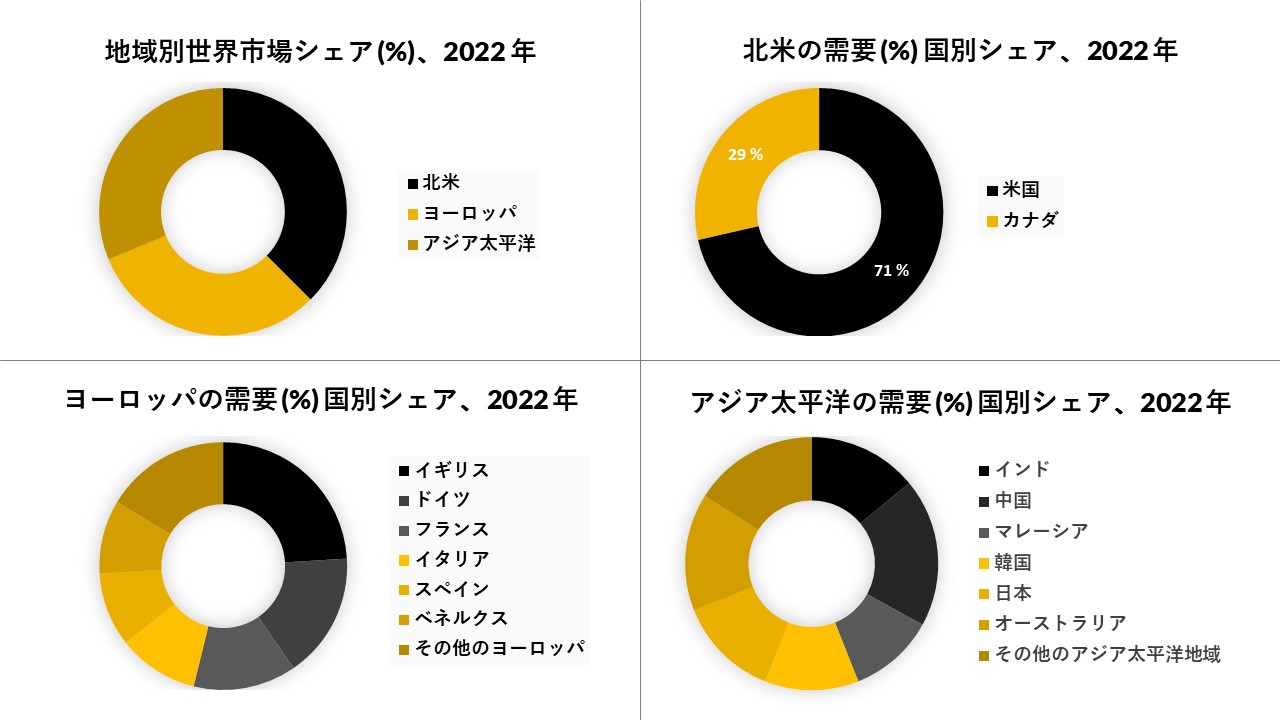
米国の医療詐欺検出市場は、予測期間中に24.47%のCAGRを記録すると予想されています

米国の医療詐欺検出市場は、予測期間中に24.47%のCAGRを記録すると予想されています。米国の医療不正検出市場の成長に起因する主な要因は、米国の医療における不正行為の増加、運用効率の向上と医療費の削減に対する圧力の高まり、および前払いレビューモデルです
National Health Care Anti-Fraud Associationによると、米国における健康保険詐欺は、消費者にとって年間約800億米ドルの費用がかかります。犯罪者は、全国の人々から利益を得ることを楽しみにしています。国のほとんどの人が健康保険に加入しているため、無料の医療や無料の相談オファーが盗まれています.
このような健康保険の不正事件は、人々の病歴に損害を与えています。数年前、犯罪者はあらゆる種類の患者識別情報と保険情報を使用していたため、医療従事者が詐欺を特定することは困難でした。このような詐欺のために、患者はより高い保険料を支払うことを余儀なくされます。したがって、米国の医療省は現在、詐欺検出技術を実装することによって、そのようなケースの削減にもっと焦点を当てています。したがって、米国の医療部門における不正行為の増加により、調査された市場は将来成長する可能性があると考えられています
主な市場動向
アプリケーションセグメントでは、保険金請求の見直しセグメントが主要なシェア
医療詐欺検出ソリューションは、ほとんどの詐欺事件が保険の請求中に発生するため、保険金請求のレビューにおいて重要な役割を果たします。全米医療詐欺防止協会(NHCAA)の見積もりによると、医療詐欺は米国で年間約680億ドルの費用がかかります。健康保険詐欺とは、保険契約者、他者、またはサービスを提供する事業体に不正な給付金を支払わせようとして、虚偽または誤解を招くような情報を健康保険会社に提供する詐欺の一種です。犯罪は、被保険者または医療サービスの提供者によって犯される可能性があります.
ほとんどの健康保険には、特定の給付金や、受け取ったサービスの種類に対する過大請求などの健康保険詐欺の慣行が含まれています。最近の米国の医療政策改革の中心的な目的は、安定した手頃な価格の健康保険へのアクセスを増やすことでした。前述の要因により、保険金請求セグメントの見直しは、米国の医療詐欺検出市場で指数関数的に成長すると予想されています
競争環境
米国の医療詐欺検出市場は中程度の競争が激しく、いくつかの主要プレーヤーで構成されています。市場シェアの面では、主要なプレーヤーのいくつかが現在市場を支配しています。医療ITの採用が進み、詐欺事件の数が増えているため、今後数年間で市場に参入する小規模なプレーヤーはほとんどいないと予想されています。市場の主要プレーヤーのいくつかは、Conduent Inc.、DXC Technology Company、EXL(Scio Health Analytics)、International Business Machines Corporation(IBM)、Mckessonなどです
このレポートを購入する理由:
- エクセル形式の市場予測(ME)シート
- 3ヶ月のアナリストサポート

北米(米国およびカナダ)、ラテンアメリカ(ブラジル、メキシコ、アルゼンチン、その他のラテンアメリカ)、ヨーロッパ(英国、ドイツ、フランス、イタリア、スペイン、ハンガリー、ベルギー、オランダおよびルクセンブルグ、NORDIC(フィンランド、スウェーデン、ノルウェー) 、デンマーク)、アイルランド、スイス、オーストリア、ポーランド、トルコ、ロシア、その他のヨーロッパ)、ポーランド、トルコ、ロシア、その他のヨーロッパ)、アジア太平洋(中国、インド、日本、韓国、シンガポール、インドネシア、マレーシア) 、オーストラリア、ニュージーランド、その他のアジア太平洋地域)、中東およびアフリカ(イスラエル、GCC(サウジアラビア、UAE、バーレーン、クウェート、カタール、オマーン)、北アフリカ、南アフリカ、その他の中東およびアフリカ)